What Event at Letter B Leads to Elongation of the Bone?
Os Tissue and the Skeletal Organization
Bone Formation and Development
Learning Objectives
Past the end of this section, you will be able to:
- Explain the function of cartilage
- List the steps of intramembranous ossification
- List the steps of endochondral ossification
- Explicate the growth activity at the epiphyseal plate
- Compare and contrast the processes of modeling and remodeling
In the early stages of embryonic development, the embryo's skeleton consists of fibrous membranes and hyaline cartilage. By the sixth or 7th week of embryonic life, the actual process of bone development, ossification (osteogenesis), begins. There are two osteogenic pathways—intramembranous ossification and endochondral ossification—but os is the aforementioned regardless of the pathway that produces it.
Cartilage Templates
Bone is a replacement tissue; that is, information technology uses a model tissue on which to lay downwardly its mineral matrix. For skeletal development, the nearly common template is cartilage. During fetal development, a framework is laid down that determines where bones will form. This framework is a flexible, semi-solid matrix produced by chondroblasts and consists of hyaluronic acid, chondroitin sulfate, collagen fibers, and water. As the matrix surrounds and isolates chondroblasts, they are called chondrocytes. Different well-nigh connective tissues, cartilage is avascular, meaning that it has no claret vessels supplying nutrients and removing metabolic wastes. All of these functions are carried on past diffusion through the matrix. This is why damaged cartilage does not repair itself equally readily as most tissues practise.
Throughout fetal development and into babyhood growth and evolution, bone forms on the cartilaginous matrix. By the time a fetus is built-in, nearly of the cartilage has been replaced with os. Some boosted cartilage will exist replaced throughout childhood, and some cartilage remains in the adult skeleton.
Intramembranous Ossification
During intramembranous ossification, compact and spongy bone develops directly from sheets of mesenchymal (undifferentiated) connective tissue. The flat bones of the face, well-nigh of the cranial bones, and the clavicles (collarbones) are formed via intramembranous ossification.
The procedure begins when mesenchymal cells in the embryonic skeleton get together together and begin to differentiate into specialized cells ((Figure)a). Some of these cells will differentiate into capillaries, while others will get osteogenic cells and and so osteoblasts. Although they will ultimately be spread out past the formation of bone tissue, early osteoblasts announced in a cluster called an ossification eye.
The osteoblasts secrete osteoid, uncalcified matrix, which calcifies (hardens) within a few days as mineral salts are deposited on it, thereby entrapping the osteoblasts within. One time entrapped, the osteoblasts become osteocytes ((Figure)b). Equally osteoblasts transform into osteocytes, osteogenic cells in the surrounding connective tissue differentiate into new osteoblasts.
Osteoid (unmineralized os matrix) secreted around the capillaries results in a trabecular matrix, while osteoblasts on the surface of the spongy bone become the periosteum ((Effigy)c). The periosteum then creates a protective layer of compact bone superficial to the trabecular os. The trabecular os crowds nearby blood vessels, which eventually condense into red marrow ((Figure)d).
Intramembranous Ossification
Intramembranous ossification follows 4 steps. (a) Mesenchymal cells group into clusters, and ossification centers form. (b) Secreted osteoid traps osteoblasts, which then become osteocytes. (c) Trabecular matrix and periosteum form. (d) Compact bone develops superficial to the trabecular os, and crowded claret vessels condense into ruby marrow.
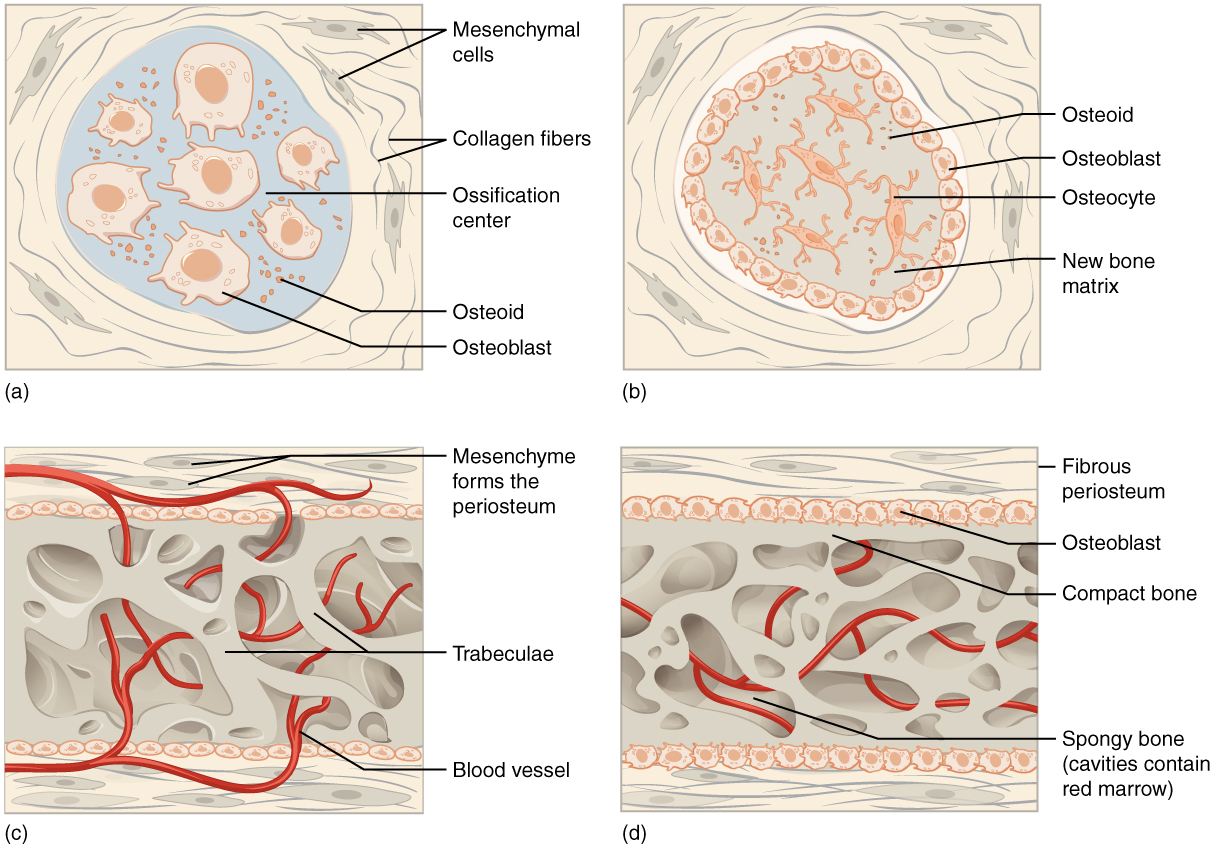
Intramembranous ossification begins in utero during fetal development and continues on into adolescence. At birth, the skull and clavicles are not fully ossified nor are the sutures of the skull closed. This allows the skull and shoulders to deform during passage through the nativity culvert. The last bones to ossify via intramembranous ossification are the flat bones of the face, which reach their adult size at the finish of the boyish growth spurt.
Endochondral Ossification
In endochondral ossification, os develops past replacing hyaline cartilage. Cartilage does not get bone. Instead, cartilage serves as a template to be completely replaced by new bone. Endochondral ossification takes much longer than intramembranous ossification. Basic at the base of operations of the skull and long bones form via endochondral ossification.
In a long bone, for case, at almost half-dozen to viii weeks after conception, some of the mesenchymal cells differentiate into chondrocytes (cartilage cells) that grade the cartilaginous skeletal forerunner of the bones ((Figure)a). Soon afterward, the perichondrium, a membrane that covers the cartilage, appears (Figure)b).
Endochondral Ossification
Endochondral ossification follows v steps. (a) Mesenchymal cells differentiate into chondrocytes. (b) The cartilage model of the future bony skeleton and the perichondrium form. (c) Capillaries penetrate cartilage. Perichondrium transforms into periosteum. Periosteal neckband develops. Primary ossification eye develops. (d) Cartilage and chondrocytes continue to grow at ends of the os. (due east) Secondary ossification centers develop. (f) Cartilage remains at epiphyseal (growth) plate and at articulation surface as articular cartilage.
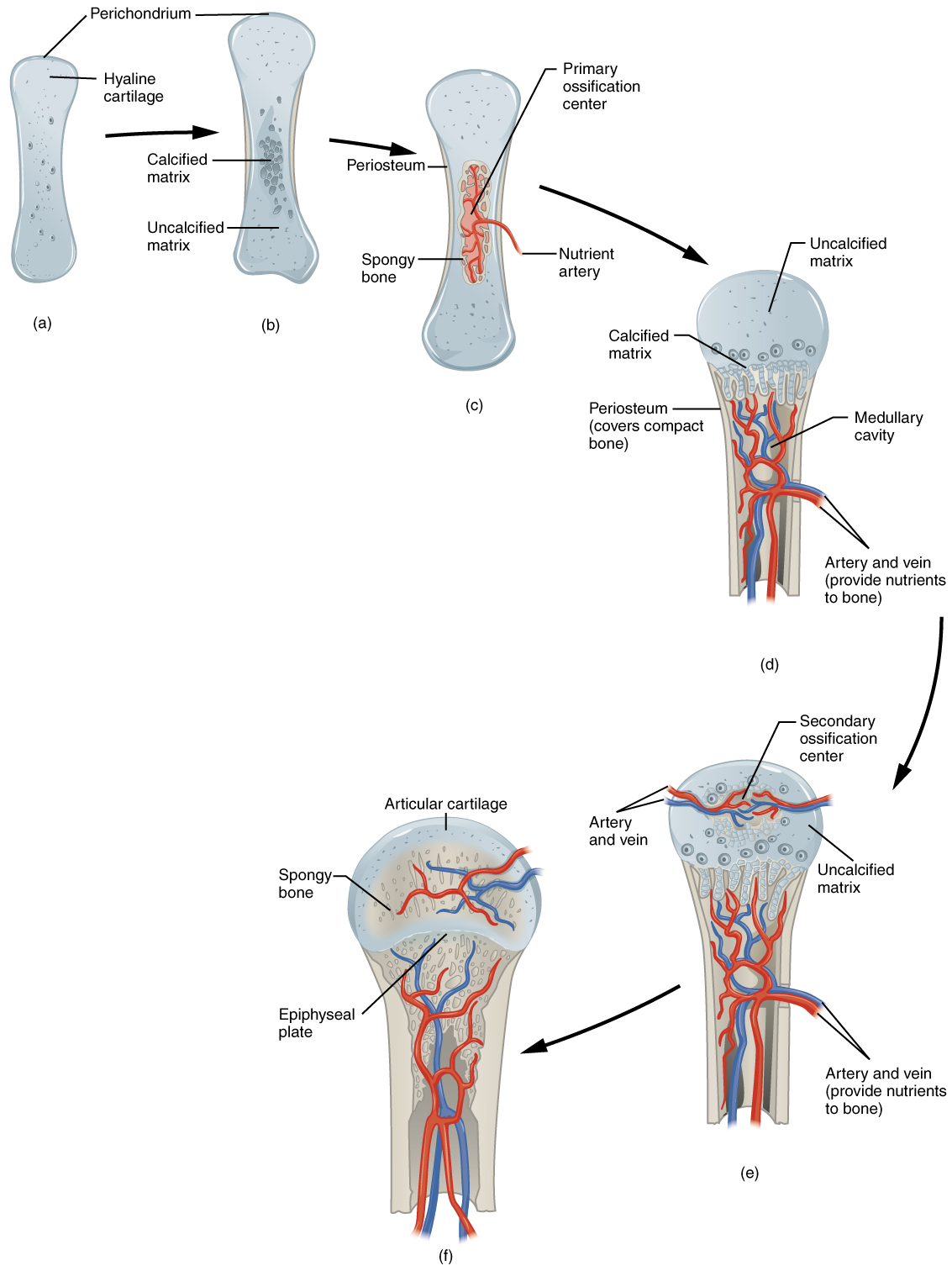
Every bit more matrix is produced, the chondrocytes in the center of the cartilaginous model grow in size. Every bit the matrix calcifies, nutrients can no longer reach the chondrocytes. This results in their death and the disintegration of the surrounding cartilage. Blood vessels invade the resulting spaces, not only enlarging the cavities but also carrying osteogenic cells with them, many of which will become osteoblasts. These enlarging spaces somewhen combine to go the medullary cavity.
As the cartilage grows, capillaries penetrate it. This penetration initiates the transformation of the perichondrium into the bone-producing periosteum. Hither, the osteoblasts form a periosteal collar of compact os around the cartilage of the diaphysis. By the second or third month of fetal life, os cell development and ossification ramps upwards and creates the primary ossification center, a region deep in the periosteal collar where ossification begins ((Figure)c).
While these deep changes are occurring, chondrocytes and cartilage continue to grow at the ends of the bone (the future epiphyses), which increases the bone's length at the same time bone is replacing cartilage in the diaphyses. Past the fourth dimension the fetal skeleton is fully formed, cartilage only remains at the articulation surface as articular cartilage and between the diaphysis and epiphysis equally the epiphyseal plate, the latter of which is responsible for the longitudinal growth of basic. Later birth, this aforementioned sequence of events (matrix mineralization, death of chondrocytes, invasion of blood vessels from the periosteum, and seeding with osteogenic cells that become osteoblasts) occurs in the epiphyseal regions, and each of these centers of activity is referred to as a secondary ossification center ((Figure)due east).
How Bones Abound in Length
The epiphyseal plate is the area of growth in a long bone. It is a layer of hyaline cartilage where ossification occurs in immature bones. On the epiphyseal side of the epiphyseal plate, cartilage is formed. On the diaphyseal side, cartilage is ossified, and the diaphysis grows in length. The epiphyseal plate is composed of four zones of cells and activity ((Figure)). The reserve zone is the region closest to the epiphyseal stop of the plate and contains small chondrocytes inside the matrix. These chondrocytes do not participate in bone growth but secure the epiphyseal plate to the osseous tissue of the epiphysis.
Longitudinal Bone Growth
The epiphyseal plate is responsible for longitudinal os growth.
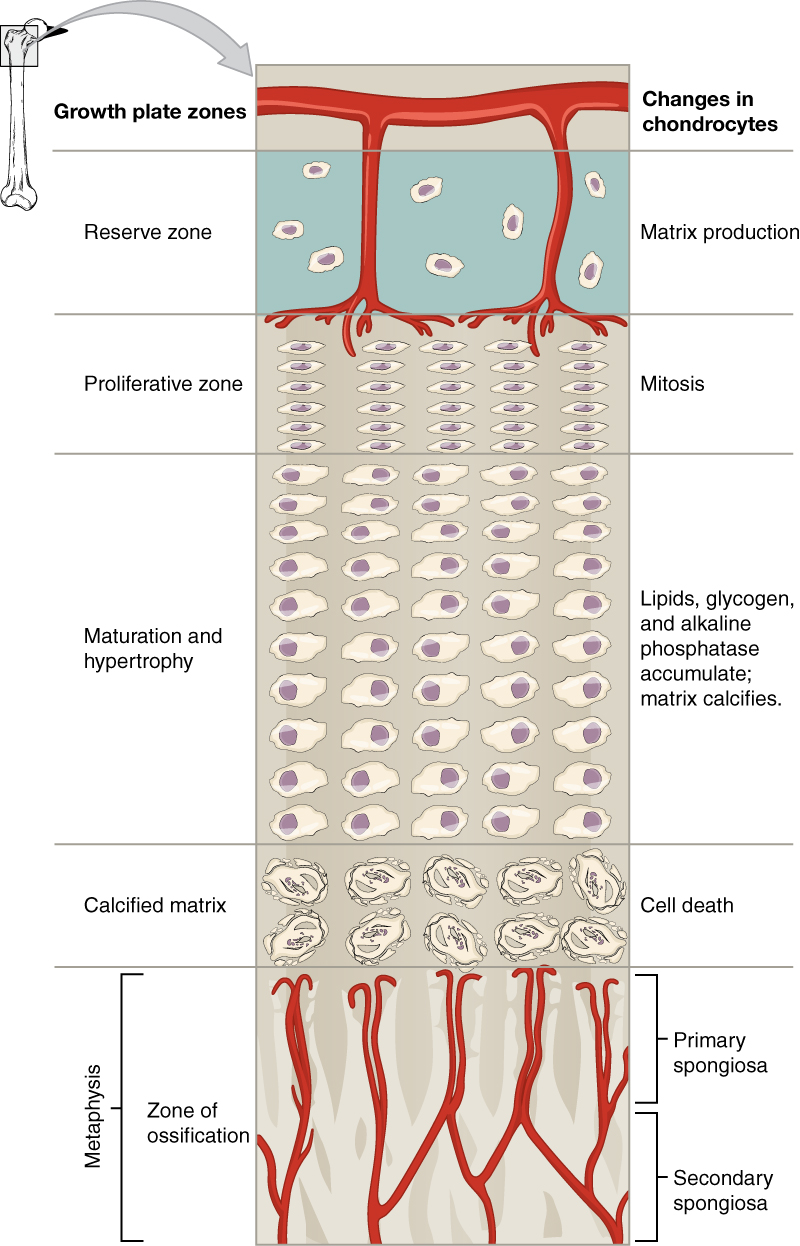
The proliferative zone is the adjacent layer toward the diaphysis and contains stacks of slightly larger chondrocytes. It makes new chondrocytes (via mitosis) to replace those that die at the diaphyseal end of the plate. Chondrocytes in the adjacent layer, the zone of maturation and hypertrophy, are older and larger than those in the proliferative zone. The more than mature cells are situated closer to the diaphyseal cease of the plate. The longitudinal growth of bone is a effect of cellular partition in the proliferative zone and the maturation of cells in the zone of maturation and hypertrophy.
Most of the chondrocytes in the zone of calcified matrix, the zone closest to the diaphysis, are expressionless because the matrix around them has calcified. Capillaries and osteoblasts from the diaphysis penetrate this zone, and the osteoblasts secrete bone tissue on the remaining calcified cartilage. Thus, the zone of calcified matrix connects the epiphyseal plate to the diaphysis. A os grows in length when osseous tissue is added to the diaphysis.
Basic go on to grow in length until early adulthood. The rate of growth is controlled past hormones, which will be discussed later. When the chondrocytes in the epiphyseal plate cease their proliferation and bone replaces the cartilage, longitudinal growth stops. All that remains of the epiphyseal plate is the epiphyseal line ((Figure)).
Progression from Epiphyseal Plate to Epiphyseal Line
As a bone matures, the epiphyseal plate progresses to an epiphyseal line. (a) Epiphyseal plates are visible in a growing bone. (b) Epiphyseal lines are the remnants of epiphyseal plates in a mature bone.
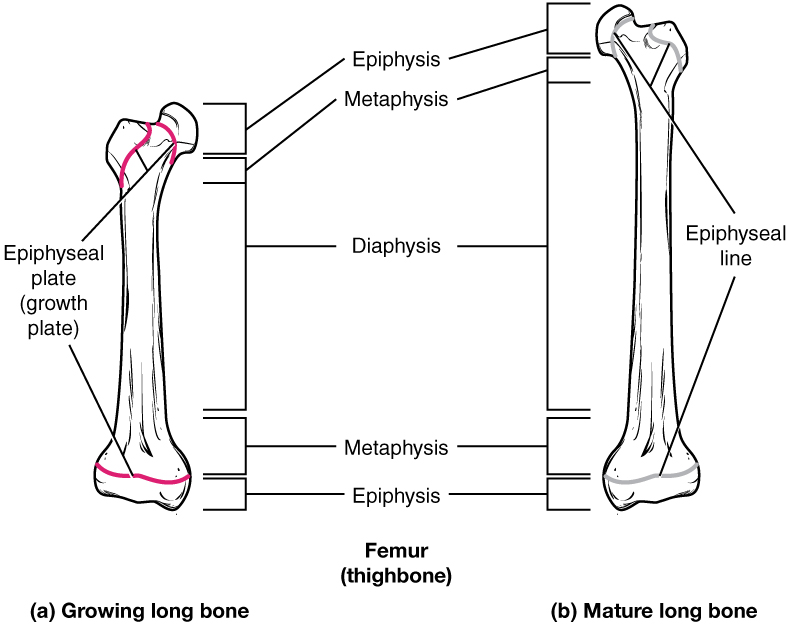
How Bones Grow in Diameter
While basic are increasing in length, they are also increasing in diameter; growth in diameter can proceed even later on longitudinal growth ceases. This is chosen appositional growth. Osteoclasts resorb quondam bone that lines the medullary cavity, while osteoblasts, via intramembranous ossification, produce new bone tissue beneath the periosteum. The erosion of onetime bone along the medullary cavity and the deposition of new bone below the periosteum not only increment the diameter of the diaphysis but also increase the diameter of the medullary cavity. This process is called modeling.
Bone Remodeling
The procedure in which matrix is resorbed on one surface of a bone and deposited on some other is known every bit bone modeling. Modeling primarily takes place during a bone'southward growth. However, in adult life, os undergoes remodeling, in which resorption of erstwhile or damaged bone takes place on the same surface where osteoblasts lay new bone to replace that which is resorbed. Injury, do, and other activities lead to remodeling. Those influences are discussed afterwards in the chapter, only fifty-fifty without injury or exercise, about v to 10 percent of the skeleton is remodeled annually just by destroying former bone and renewing information technology with fresh bone.
Diseases of the…
Skeletal System Osteogenesis imperfecta (OI) is a genetic affliction in which bones do not class properly and therefore are fragile and break easily. Information technology is besides called breakable os disease. The affliction is nowadays from birth and affects a person throughout life.
The genetic mutation that causes OI affects the body'south production of collagen, i of the critical components of bone matrix. The severity of the disease can range from balmy to severe. Those with the most severe forms of the affliction sustain many more fractures than those with a mild form. Frequent and multiple fractures typically lead to os deformities and short stature. Bowing of the long basic and curvature of the spine are also common in people afflicted with OI. Curvature of the spine makes breathing difficult considering the lungs are compressed.
Because collagen is such an important structural protein in many parts of the torso, people with OI may also experience fragile peel, weak muscles, loose joints, easy bruising, frequent nosebleeds, breakable teeth, blue sclera, and hearing loss. At that place is no known cure for OI. Treatment focuses on helping the person retain as much independence equally possible while minimizing fractures and maximizing mobility. Toward that terminate, safe exercises, similar swimming, in which the trunk is less likely to experience collisions or compressive forces, are recommended. Braces to support legs, ankles, knees, and wrists are used as needed. Canes, walkers, or wheelchairs can as well help compensate for weaknesses.
When basic do intermission, casts, splints, or wraps are used. In some cases, metallic rods may be surgically implanted into the long bones of the arms and legs. Research is currently beingness conducted on using bisphosphonates to treat OI. Smoking and being overweight are especially risky in people with OI, since smoking is known to weaken bones, and actress body weight puts additional stress on the bones.
Watch this video to see how a os grows.
Chapter Review
All bone germination is a replacement procedure. Embryos develop a cartilaginous skeleton and various membranes. During evolution, these are replaced by bone during the ossification process. In intramembranous ossification, os develops direct from sheets of mesenchymal connective tissue. In endochondral ossification, os develops by replacing hyaline cartilage. Action in the epiphyseal plate enables bones to grow in length. Modeling allows basic to grow in diameter. Remodeling occurs as bone is resorbed and replaced by new os. Osteogenesis imperfecta is a genetic disease in which collagen product is altered, resulting in fragile, brittle basic.
Review Questions
Why is cartilage slow to heal?
- considering it somewhen develops into os
- because information technology is semi-solid and flexible
- because it does not have a blood supply
- considering endochondral ossification replaces all cartilage with os
Why are osteocytes spread out in bone tissue?
- They develop from mesenchymal cells.
- They are surrounded by osteoid.
- They travel through the capillaries.
- Formation of osteoid spreads out the osteoblasts that formed the ossification centers.
In endochondral ossification, what happens to the chondrocytes?
- They develop into osteocytes.
- They die in the calcified matrix that surrounds them and form the medullary cavity.
- They grow and form the periosteum.
- They group together to form the master ossification center.
Which of the following basic is (are) formed by intramembranous ossification?
- the metatarsals
- the femur
- the ribs
- the flat bones of the cranium
Bones grow in length due to activity in the ________.
- epiphyseal plate
- perichondrium
- periosteum
- medullary crenel
Bones grow in diameter due to bone germination ________.
- in the medullary cavity
- beneath the periosteum
- in the epiphyseal plate
- within the metaphysis
Which of the post-obit represents the correct sequence of zones in the epiphyseal plate?
- proliferation, reserved, maturation, calcification
- maturation, proliferation, reserved, calcification
- calcification, maturation, proliferation, reserved
- calcification, reserved, proliferation, maturation
Critical Thinking Questions
In what ways practise intramembranous and endochondral ossification differ?
In intramembranous ossification, bone develops directly from sheets of mesenchymal connective tissue, but in endochondral ossification, bone develops past replacing hyaline cartilage. Intramembranous ossification is complete by the cease of the boyish growth spurt, while endochondral ossification lasts into young adulthood. The apartment bones of the face, most of the cranial basic, and a good bargain of the clavicles (collarbones) are formed via intramembranous ossification, while basic at the base of operations of the skull and the long basic form via endochondral ossification.
Considering how a long bone develops, what are the similarities and differences betwixt a primary and a secondary ossification center?
A single primary ossification heart is present, during endochondral ossification, deep in the periosteal collar. Like the chief ossification center, secondary ossification centers are present during endochondral ossification, but they form later, and there are ii of them, 1 in each epiphysis.
Glossary
- endochondral ossification
- process in which bone forms by replacing hyaline cartilage
- epiphyseal line
- completely ossified remnant of the epiphyseal plate
- intramembranous ossification
- process by which bone forms directly from mesenchymal tissue
- modeling
- process, during bone growth, past which bone is resorbed on ane surface of a bone and deposited on another
- ossification
- (besides, osteogenesis) os formation
- ossification center
- cluster of osteoblasts found in the early on stages of intramembranous ossification
- osteoid
- uncalcified os matrix secreted by osteoblasts
- perichondrium
- membrane that covers cartilage
- master ossification heart
- region, deep in the periosteal collar, where os development starts during endochondral ossification
- proliferative zone
- region of the epiphyseal plate that makes new chondrocytes to supervene upon those that die at the diaphyseal end of the plate and contributes to longitudinal growth of the epiphyseal plate
- remodeling
- process by which osteoclasts resorb sometime or damaged bone at the same fourth dimension as and on the same surface where osteoblasts form new bone to supervene upon that which is resorbed
- reserve zone
- region of the epiphyseal plate that anchors the plate to the osseous tissue of the epiphysis
- secondary ossification center
- region of bone development in the epiphyses
- zone of calcified matrix
- region of the epiphyseal plate closest to the diaphyseal finish; functions to connect the epiphyseal plate to the diaphysis
- zone of maturation and hypertrophy
- region of the epiphyseal plate where chondrocytes from the proliferative zone grow and mature and contribute to the longitudinal growth of the epiphyseal plate
Source: https://opentextbc.ca/anatomyandphysiologyopenstax/chapter/bone-formation-and-development/
0 Response to "What Event at Letter B Leads to Elongation of the Bone?"
Post a Comment